International Journal of Epidemiology And Public Health Research
OPEN ACCESS | Volume 9 - Issue 1 - 2026
ISSN No: 2836-2810 | Journal DOI: 10.61148/2836-2810/IJEPHR
J. S. Craven
Retired Corporate Research Fellow, Unaffiliated.
*Corresponding author: J. S. Craven, Retired Corporate Research Fellow, Unaffiliated.
Received: March 10, 2026 | Accepted: March 17, 2026 | Published: March 23, 2026
Citation: J. S. Craven., (2026) “Are the Choices We Make Independent of the Influence of Pollution?”. International Journal of Epidemiology and Public Health Research, 9(2); DOI: 10.61148/2836-2810/IJEPHR/193.
Copyright: © 2026. J. S. Craven. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
The picture of Bruce Willis appeared on December 2025 PEOPLE magazine’s cover with the headline that he was suffering from dementia. This “jolted” the author of this article since they grew up in the same twin communities of Carney’s Point - Penns Grove, Salem County, New Jersey. Author was familiar with others from area, who suffered from dementia from their late 40s. Dementia is broad term for neurocognitive disorders that impair memory, thinking, and daily function. Common types include Alzheimer’s, vascular dementia, Lewy body dementia, and frontotemporal dementia. Bruce Willis was known to be a heavy drinker and smoker of weed as a young adult, and there is a link between heavy drinking, smoking, and middle age obesity with propensity for dementia. There is also a link between pollution and dementia, which raises questions (1) whether choices to drink, smoke, and over consume are independent of the influence of exposure to pollution, (2) is pollution exposure prerequisite to other contributing factors leading to dementia. A search via “AI” revealed “No, choices are not independent of the influence of pollution”. Research indicates that higher levels of pollution impair cognitive function, leading to more mistakes and higher stress levels.” MIT Management Sloan School on February 3, 2020 addressing “The psychological, economic, and social costs of air pollution” stated that “Air pollution’s destructive consequences go beyond breathing. Research links it to anxiety, dementia, missed work, criminal behavior, and more.” The Carney’s Point – Penns Grove twin communities were created by DuPont managers to support for a century its largest chemical manufacturing plant. This plant has been proven to be a huge air polluter and a huge solid and liquid waste disposer throughout its history. This article will delve into significant aspects of plant’s waste emissions, review related assessments on links to dementia, and compare pollution vs dementia in the world’s three largest polluting countries - China, USA and India.
dementia
Hollywood Reporter on January 28, 2026 discussed famous American actor Bruce Willis’s frontotemporal dementia (FTD). He is 70 years old and grew up in Carneys Point, New Jersey within a few miles of the E.I. DuPont de Nemours & Company, Inc. manufacturing complex nearby in Carneys Point and Deepwater, Salem County, New Jersey.
Carneys Point Plant [1] was established in 1892 and was critical for producing smokeless gunpowder, particularly during the Spanish American War and World War I. It employed 27,000 employees at its peak during WWI. Smokeless powder operations continued under the DuPont Petrochemicals Department until the plant was closed in the late 1970s.
In 1916 on the extended property to the south, organic chemicals and dyes began production and later became a major site for producing Freon, leaded gasoline, aniline dye, Teflon, Stain Master. Chambers Works became the name of the site in 1944. In 1917, DuPont, seeking to end reliance on German dyes, began construction of a dye works and the Jackson dye research laboratory at Deepwater. The site produced some of DuPont's most important chemicals, particularly tetraethyl lead (TEL), used as an anti-knock agent in gasoline. Deepwater was the only plant in the Western hemisphere producing TEL up to 1948, when it accounted for the bulk of Deepwater's production. During the 1950s and 1960s, the site was the center of DuPont's highly profitable dye operations. With 6,500 employees working in more than 500 buildings, Deepwater was the largest individual chemical plant in the world's largest chemical company. In 1926 its chemists collaborated with researchers from General Motors to develop a process for making the gasoline anti-knock additive, tetraethyl lead or TEL. A few years later Jackson researchers developed a successful process for the commercial production of Freon®, a chlorofluorocarbon gas used as a refrigerant and aerosol propellant. Extended research into Freon derivatives yielded Jackson Laboratory's most famous discovery of a new, slippery and remarkably durable material later known as Teflon®. Jackson Laboratory as part of the department Organic Chemicals (Orchem) in 1931 was involved in improving neoprene synthetic rubber. DuPont's dyestuffs research peaked in the 1950s, with Jackson chemists developing suitable dyes for DuPont's Orlon and Dacron synthetic fibers. DuPont left the dye business and restructured its Organic Chemicals Department in the early 1980s.
The Carney’s Point and Chambers Works Plants are located along the Delaware River in Salem County, New Jersey. A large, extensive incineration and waste treatment plant was installed in the 1970s and ultimately a Waste Treatment Business for non-DuPont wastes followed. Prior to this WWTP, hazardous liquid waste [2] was discharged through miles of on-site unlined earthen ditches that discharged into the Delaware River (Boutten and Henby Creeks) and/or stored in three on-site unlined ponds and lagoons. Hazardous solid waste was buried in on-site landfills or buried underground in drums (waste solvents like benzene and cyanogens) inside plastic bags. Historical operations left a significant environmental footprint, including contamination of groundwater and soils with PCBs, heavy metals like lead and mercury and “forever chemicals” (PFAs). During the 1950s, the DuPont Chambers Works was a major source of both water and air pollution, characterized by the large scale, early and largely unregulated, use and release of PFAs (specifically PFOA/C8) and other industrial chemicals. Pungent odors and nauseating gases were well known as was in-plant “Teflon flu”. Surrounding area of Deepwater was subjected to airborne pollutants. PFOA was often shipped to the factory pre-mixed with water to reduce, but not eliminate, the release of dust from smokestacks. At its peak Chambers Works had 225 smokestacks [3] nominally discharging about 150 feet aboveground level. These stacks discharged chemical waste gases like aqueous hydrochloric acid, sulfuric acid, ammonia, and process hazardous dusts. 4x12 shift operation was infamous for a heavy white cloud hovering over the southern portion of the site visible from the Delaware Memorial Bridge formed by the airborne mixing of sulfuric acid fumes from oleum reaction “drownings” and ammonia fumes from the amination areas. A resulting visible white dust, ammonium sulfate was formed.
The plant was a major source of dyes, organic chemicals, and in the 1940s a legacy of radiation and fluorine. In the 1950s with minimal federal regulations the site was considered one of the most heavily contaminated in New Jersey. In the TEL operating area workers were routinely monitored for lead accumulation in their blood. In the dyes operating area workers were routinely monitored for mercury accumulation in their blood. High measured levels led to inability to work in these area until levels regained low values.
Documentation by the National Institute of Health (NIH) [4] and the World Health Organization (WHO) indicates that PFAs, pesticides, lead and mercury are primary triggers enabling the onset of dementia and various other forms of mental health diseases. A search of “AI” for the “long term impact of childhood exposure to Tetra Ethyl Lead, also known as looney gas, on aging mental health provided similar result.
Air pollution, particularly fine particulate matter (PM2.5), is a significant modifiable risk factor for dementia [5], causing over 625,000 deaths annually. The highest total burdens are in heavily polluted, populous countries like China, India, and the United States, while high-income countries with aging populations see the highest per capita rates. The mechanism is that fine pollutants penetrate lungs, enter bloodstream, and cause systemic inflammation and brain tissue damage. Living within 50 meters of a major road with high traffic pollution increases dementia risk by 12%. 36% of the world’s population is exposed to levels of PM2.5 pollution above the least stringent target of 35ug/m3. While 99% of the world’s population lives in areas with poor air quality, older, urban populations in industrial nations are most vulnerable. Air pollution is considered a key, potentially modifiable risk factor for dementia alongside traditional risks like tobacco and diet.
Bruce Willis and Dementia
A December 2025 People Magazine cover headline explained that famous Hollywood actor Bruce Willis had for the past five years dementia, type FTD. Bruce grew up in the connecting towns between Penns Grove and Pennsville, which included the villages of Carneys Point and Deepwater, a total distance of less than 10 miles. These towns border the Delaware River near the now twin Delaware Memorial Bridges. Between these towns and the River was the contiguous 1,500 acre DuPont Carneys Point smokeless gunpowder plant and Chambers Works. At one time of the 7,000 families in Salem County, 5,000 of these families had at least one person working at these plants. Peak employment at Chambers Works during WWII was 12,000 employees.
Preliminary engineering research on the connection of Bruce Willis’s dementia, and known waste emissions from Chambers Works provided the following pertinent information. NIH and WHO documents indicate PFAS, pesticides, lead and mercury are all triggers for dementia. Published New Jersey court documents conclusively show that DuPont Chambers Works knowingly disposed of these chemicals for up to a half century to protect their profits before the Clean Water Act, before RCRA, before Right-to-Know. The residual operating Chambers Works now has a few hundred employees, maintains 27 interrupter wells circling the plant to monitor hazardous chemical leakage underground and has been fined over a couple billion dollars for long term clean-up. Chambers Works historical major money making products were Tetra Ethyl Lead (also known as looney gas), Freon, Teflon, Stain Master, and a variety of synthetic organic dyes and chemicals, such as aniline dyes (linked to cancer). All of these products are now banned products federally. Chambers Works is no longer part of DuPont.
Until about 1980 production wastes not vented to the atmosphere were either buried on-site or disposed via miles of on-site unlined earthen trenches across the site via outfalls to the Delaware River. Lead waste from TEL and PFA waste from Freon and Stain master are obvious. What might be less obvious is that mercury sulfate was extensively used as a catalyst (Lewis Acid) in the manufacture of synthetic organic anthraquinone dyes. Salem County, New Jersey, where these plants are located, is 27% swamp land. To make the county land useful, bottoms from local creeks and rivers were used to “dry out” the swamp land. The land these plants were built on was previously known as "Skunks Misery" [1]. Local youth waded into the Delaware River down current from the sites near the bridges and on the shore of the once famous Riverview Beach Park. Youth would sink up to their knees in "gunk". There were no warning signs to “keep out”.
A search of "AI" provided a description of what was in the "gunk".
“During the 1950s, the Delaware River in the vicinity of the Chambers Works in Deepwater, NJ was heavily contaminated [6] with industrial and sewage pollution, described as a “stinking mess”. The area, a major chemical manufacturing hub, saw extensive, largely unregulated discharges of chemical wastes, including PFAs (forever chemicals), radioactive materials, and other hazardous byproducts. Historical manufacture resulted in the contamination of groundwater and soil with various organic and inorganic (heavy metals) constituents, including PCBs. The river water essentially had zero dissolved oxygen and fish kills were common. This area was part of the region known for “South Jersey Mud” with thick, heavily polluted, “Tidal Muck” common along the tributaries. The era was marked by a “code of silence” regarding the environmental impact, as the plant was a major employer and the pollution was accepted as a consequence of economic growth.
Locals were primarily blue-collar workers (1st, 2nd, 3rd generation immigrants) in Carneys Point and Deepwater living in DuPont provided village bungalow homes (asbestos siding and asbestos linoleums) managed by a DuPont quartermaster until the 1950s. Enterprising local residents sometimes fed off the swamp land catfish and muskrats. Both are bottom feeders where wasted lead and mercury, etc., would settle and accumulate. Self-grown tomatoes, corn, lima beans, carrots and asparagus were grown in local available soil.
An article in CELEBSTONER February 18, 2023 by Steve Bloom provided the information that Bruce Willis as a teenager was a heavy drinker and enjoyed smoking weed. He often lived on pizza and beer and eventually joined AA. The Alzheimer’s Organization [7] states that evidence shows that excessive alcohol consumption increases a person’s risk of dementia. Drinking alcohol is linked to reduced volume of the brain’s white matter, which helps transmit signals between different brain regions. Heavy drinking over time can lead to sharp decline in thinking skills and memory losses people age. The Alzheimer’s Association further indicates heavy drinkers and smokers develop Alzheimer’s disease years earlier than people with Alzheimer’s who do not drink or smoke heavily.
Dementia Overview
The National Institute on Aging [4], a component of the National Institutes of Health (NIH), is a leading United States federal funder of research on dementia [1]. It provide the following information on dementia and its causes.
Frontotemporal disorders (Bruce Willis) are forms of dementia caused by a family of neurodegenerative brain diseases collectively called frontotemporal lobar degeneration. They primarily affect the frontal and temporal lobes of the brain, rather than the widespread shrinking and wasting away (atrophy) of brain tissue seen in Alzheimer's disease.
A HEALTHSPAN article in 2024 about heavy metals exposure and neurotoxicity provided the following take home points:
The evidence linking various metals to neurological disorders is both compelling and concerning. Mercury and lead are well-documented neurotoxins that contribute to significant cognitive decline and the development of neurodegenerative diseases like AD. Aluminum's association with amyloid plaques further underscores its role in neurodegeneration. Emerging research on arsenic and cadmium reveals their potential to disrupt protein function and neurotransmitter balance, leading to both cognitive and psychiatric disorders. These findings highlight the urgent need for continued research and public health initiatives to mitigate exposure to these harmful metals and protect neurological health.
Since 1 June 2020, As, Cd, Hg, and Pb have been considered among the 10 most harmful chemicals to human health by the World Health Organization, which provided risk management recommendations to protect humans from their harmful effects. Consistent with this, in 2022, the U.S. Agency for Toxic Substances and Disease Registry included As, Pb, Hg, and Cd within the top 10 substances showing the most significant toxic (known or suspected) effects in humans. In fact, in recent decades, there has been an increase in contamination by toxic metals due to their growing applications in mining, manufacturing, farming, industrial discharge, and technology. In addition to anthropogenic activities, these elements are naturally introduced into the environment thanks to events such as volcanic eruptions and rock weathering. Exposure to toxic metals occurs through diverse modes, including ingestion through diet, which represents the most relevant route, inhalation, and, occasionally, dermal absorption, while parameters such as speciation, dose, and duration of exposure can influence the effects, and the consequent toxicity, of these elements in humans. Physio-chemical soil properties, such as pH, redox potential, soil texture, organic matter content, and the presence of iron and manganese oxides and ions in the soil solution, may influence the bioavailability of metals and their capacity to transfer and accumulate in both edible and inedible parts of plants and, therefore, enter food chains. Being non-essential elements for living organisms and not subject to biodegradation, often with a long half-life, they can accumulate in the human body, causing harmful health effects. Importantly, they may cross the blood–brain barrier (BBB) and accumulate in the brain or, alternatively, enter the CNS via the olfactory pathway. Figure 1 below provides schematic representation of the sources of contamination and exposure routes of toxic metals. Abbreviations: Al: aluminum; As: arsenic; Cd: cadmium; Hg: mercury; Pb: lead.
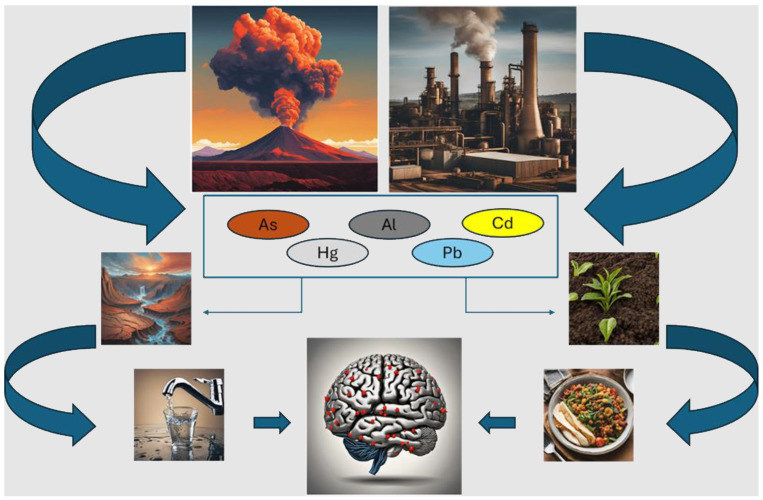
Dementia in world’s leading polluter countries
Exposure to ambient PM2.5 pollution has been linked to multiple adverse health effects. Additional effects have been identified in the literature and there is a need to understand its potential role in high prevalence diseases. In response to recent indications of PM2.5 as a risk factor for dementia, examination of the evidence by systematically reviewing the epidemiologic literature, in relation to exposure from ambient air pollution, household air pollution, secondhand smoke, and active smoking. A preliminary exposure-response functions was developed, estimating the uncertainty, and discussing sensitivities and model selection. Estimates indicate the likely impact to be 2.1 M (1.4 M, 2.5 M; 5%–95% confidence) global incident dementia cases and 0.6 M (0.4 M, 0.8 M) deaths attributable to ambient PM2.5 pollution in 2015. This implies a combined toll from morbidity and mortality of dementia of 7.3 M (5.0 M, 9.1 M) lost disability-adjusted life years. China, Japan, India, and the United States had the highest estimated total burden, and the per capita burden was highest in developed countries with large elderly populations. Compared to 2000, most countries in Europe, the Americas, and Southern Africa reduced the burden in 2015, while other regions had a net increase. Based on a recent systematic review of cost of illness studies for dementia, estimates imply economic costs of US$ 26 billion worldwide in 2015. Based on this estimation, ambient PM2.5 pollution may be responsible for 15% of premature deaths and 7% of DALYs associated with dementia.
The Figure below provides a pictorial of the effects of air pollutants on brain health.
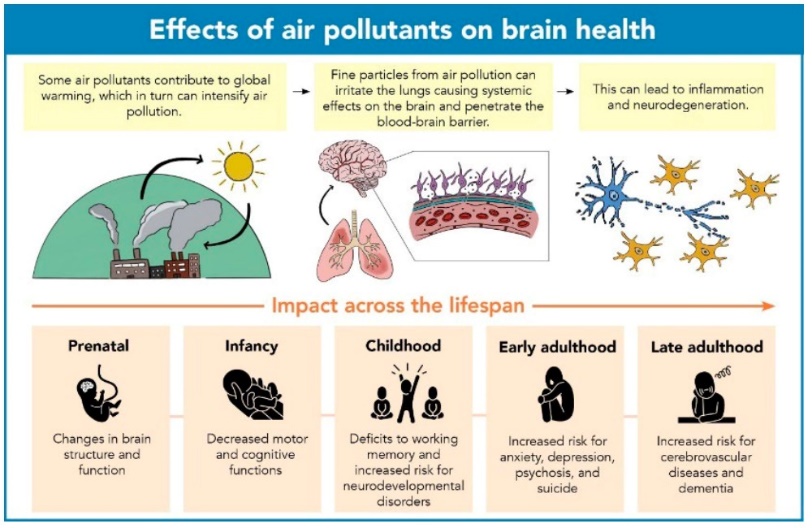
How deadly is air pollution?
01:08
A CNN article September 28, 2016 by Jacqueline Howard stated that scientists have long known that breathing dirty air can be bad for your health, including your brain health.
A study, published in the medical journal BMJ Open, weighs just how much exposure to high amounts of air and noise pollution could be linked with an increased risk of dementia.
The study found that among older adults in London, those living in areas with the highest amount of annual air pollution concentration in the region were at a subsequent higher risk of dementia compared with those living in areas with the lowest amount.
Specifically, those in the top fifth areas of exposure “were 40% more likely to be diagnosed with dementia in the study” than those in the bottom fifth, even after adjusting for other risk factors like smoking or socioeconomic status, said Iain Carey, a senior lecturer of epidemiology in the Population Health Research Institute at St. George’s University of London, who was lead author of the paper.
Conclusion
The author of this article was personally energized to understand the relationship of the dementia experienced by so many of the people he knew in the Salem County area near the DuPont industrial complex. Bruce Willis’s diagnosis was a red flag that required follow-up. For several days the author pondered how to present his research findings. Ultimately the concept that living and working in a heavily polluted environment dominated behavioral patterns and choices made. The preponderant locales for worldwide cases of dementia are in heavily industrialized blue collar areas, where every aspect of lives from birth to old age are directly affected by exposure to the polluted surrounding environment. As such everyday choices are affected. The interaction with the developing person from childbirth with pollution affects fundamental choices in unknowing ways. Stress, alcohol consumption, smoking, over consumption of food, etc. are not surprising reactions.
The data presented in this article unquestionably links industrial pollution from fine particulates to heavy metals, etc. to dementia. It's a very high probability that the dementia now being experienced by Bruce Willis was caused by childhood exposure to heavy metals and/or other industrial wastes disposed from the Chambers Works site including fine particulate (PM2.5 micron) air emissions.
A quick "AI" search of India and dementia showed that 7.5% of all adults over the 60 years old have dementia and this is expected to double over the next generation. "AI" also indicates that India has a huge lead and mercury disposal problem. Similar to what happened in Salem County in the middle twentieth century, Narendra Modi, Prime Minister of India in the 21st century, has stated publically that nothing must stop India’s industrial growth. In December Delhi’ AQI was 600 times higher than safe to breath! This is the same outlook DuPont and the Carney’s Point – Penns Grove twin communities had for the Chambers Works complex for its first 100 years! A “Code of Silence”. Sacrifice the working community for profits and economic success! Healthcare costs worldwide are now 10% of global GNP. Where will it peak?