Clinical Case Reports and Clinical Study
OPEN ACCESS | Volume 13 - Issue 1 - 2026
ISSN No: 2766-8614 | Journal DOI: 10.61148/2766-8614/JCCRCS
Dr H.Boudhar, Dr S.tarek, Pr M.lahjaouj, Pr M.loudghiri, Pr W.Bijou, Pr Y.Oukessou, Pr R.L. Abada, Pr S.Rouadi, Pr M.Roubal, Pr M.Mahtar
ENT head and neck surgery department, 20 august hospital, Ibn rochd university hospital, Faculty of medicine and pharmacy, Hassan II university Casablanca, Morocco.
*Corresponding author: Hajar Boudhar, ENT head and neck surgery department, 20 august hospital, Ibn rochd university hospital, Faculty of medicine and pharmacy, Hassan II university Casablanca, Morocco.
Received: March 05, 2026 | Accepted: March 11, 2026 | Published: March 18, 2026
Citation: H.Boudhar, S.tarek, M.lahjaouj , M.loudghiri, W.Bijou, Y.Oukessou, R.L. Abada, S.Rouadi, M.Roubal, M.Mahtar. (2026) “Predictive Factors of Hearing Recovery after Tympanoplasty in Chronic Otitis Media” Clinical Case Reports and Clinical Study, 13(2); DOI: 10.61148/2766-8614/JCCRCS/233.
Copyright: © 2026 Hajar Boudhar. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Chronic otitis media (COM) is a persistent inflammatory condition of the middle ear that can cause significant hearing loss and serious complications. Surgical treatment aims to eradicate the disease and restore auditory function. The objective of this study was to analyze the anatomical and functional prognostic factors influencing postoperative outcomes in patients operated on for COM.
Materials and Methods
This was a retrospective descriptive and analytical study including 60 patients operated on for COM in the Department of Otorhinolaryngology and Head and Neck Surgery at Ibn Rochd University Hospital, Casablanca, between January 2021 and December 2023. Clinical, audiometric, operative, and follow-up data were analyzed using SPSS software, with a significance level set at p < 0.05.
Results
The mean age of patients was 33.9 ± 14.4 years, with a slight female predominance. Chronic otorrhea and hearing loss were the most common symptoms. Non-cholesteatomatous COM accounted for 53.3 % of cases, and the cholesteatomatous form for 46.7 %. Ossicular chain involvement was found in 70 %, mainly incus erosion. Closed tympanoplasty was performed in 65 % of cases. Anatomical results were satisfactory in 83.3 %, with stable cavity healing in 91.7 %. The mean hearing gain was 12.1 dB, with a significant reduction in the air-bone gap (p < 0.05). Better outcomes were obtained in non-cholesteatomatous COM and in cases with an intact ossicular chain. Significant prognostic factors included the type of COM, surgical technique, and ossicular status.
Conclusion
Surgery for chronic otitis media provides favorable anatomical and functional outcomes, particularly when the disease is treated early and ossicular integrity is preserved. Identifying preoperative prognostic factors is crucial to optimize surgical strategy and improve hearing rehabilitation outcomes.
Chronic otitis media – Tympanoplasty – Cholesteatoma – Prognostic factors – Hearing results – Ossiculoplasty
Chronic otitis media is a common condition with potentially serious functional and, at times, life-threatening consequences. It constitutes a major public health problem in developing countries, due to delayed diagnosis, difficulties in accessing specialized care, and the risk of intratemporal or intracranial complications [1,2]. Persistent inflammation of the middle ear mucosa leads to irreversible damage to the tympano-ossicular system, responsible for a frequently mixed hearing loss and a reduced quality of life [3,4].
Chronic cholesteatomatous otitis media (CCOM) is the most aggressive form, characterized by the presence of invasive keratinizing epithelium capable of eroding nearby bony structures. Its progression is marked by frequent recurrences and complications such as labyrinthitis, facial paralysis, or intracranial abscesses [5,6]. Treatment is based on otologic surgery, which aims both to eradicate the disease and to restore hearing. However, the prognosis depends on multiple factors: the extent of the cholesteatoma, the condition of the ossicular chain, eustachian tube function, the presence of complications, and the quality of the tympano-ossicular reconstruction [7–9].
Several classifications have been proposed to standardize the description of the condition and to guide surgical prognosis, notably those of STAMM [10], EAONO/JOS [11], and SAMEO-ATO [12]. In this context, the evaluation of prognostic audiometric and anatomical factors in chronic otitis media is essential for predicting functional outcomes and guiding therapeutic strategy.
This study aims to analyze the prognostic factors influencing anatomical and auditory outcomes following surgery for chronic otitis media, based on a series of patients operated on in the Department of Otorhinolaryngology and Head and Neck Surgery at the Ibn Rochd University Hospital in Casablanca.
Materials and Methods:
This was a descriptive and analytical retrospective study conducted in the Department of Otorhinolaryngology and Head and Neck Surgery at the 20 Août 1953 Hospital, Ibn Rochd University Hospital in Casablanca, over a three-year period from January 2021 to December 2023.
All patients, both adults and children, who underwent surgery for chronic otitis media (COM) with or without cholesteatoma and who had complete clinical and audiological records were included. Cases with hearing loss of another etiology (traumatic, congenital, or tumoral) or with incomplete post-operative follow-up were excluded.
Data collected from medical and surgical records included epidemiological parameters (age, sex, otological history, affected side); clinical characteristics (otorrhea, otalgia, hearing loss, vertigo, associated complications); pre- and post-operative audiometric results, expressed as Pure-Tone Average (PTA) and Air-Bone Gap according to AAO-HNS recommendations; and surgical data (type of otitis - cholesteatomatous or not, mucosal status, ossicular involvement, surgical technique - canal wall up or canal wall down, and type of ossicular reconstruction according to the SAMEO-ATO classification [12]).
Post-operative follow-up allowed for the evaluation of anatomical results (tympanic membrane integrity, recurrence, complete cavity epithelialization) and auditory results at 6 and 12 months.
Quantitative variables were expressed as means ± standard deviation, and qualitative variables as percentages. Associations between prognostic factors and functional outcomes were tested using the Chi-square test or Student's t-test, with a significance threshold set at p < 0.05.
The study was conducted in compliance with data confidentiality and in accordance with the ethical principles of the Declaration of Helsinki.
Results:
The study included 60 patients who underwent surgery for chronic otitis media (COM) in the Department of Otorhinolaryngology and Head and Neck Surgery at the 20 Août 1953 Hospital, Ibn Rochd University Hospital in Casablanca, between January 2021 and December 2023. The mean age of the patients was 33.9 ± 14.4 years, with a range from 7 to 75 years. The study population showed a slight female predominance, with a male-to-female sex ratio of 0.9. The condition was unilateral in 95% of cases, predominantly on the right side (55%).
Clinically, chronic otorrhea was the most frequent reason for consultation, observed in 85% of patients, followed by hearing loss in 80%, otalgia in 25%, and tinnitus in 15%. A history of recurrent acute otitis media was found in 40% of patients, while 6.6% had a family history of chronic otitis, suggesting a possible genetic or environmental susceptibility.
Preoperative audiometric data revealed a mean hearing loss of 42.1 dB, with a mean air-bone gap of 32.7 dB. The most frequently observed type of hearing loss was mixed (60%), followed by conductive (30%) and sensorineural (10%) forms. These results reflect the predominance of advanced tympano-ossicular lesions, often associated with cochlear changes secondary to chronic inflammation.
Intraoperative exploration revealed cholesteatomatous chronic otitis media (C-COM) in 46.7% of cases and a non-cholesteatomatous form (NC-COM) in 53.3%. Ossicular involvement was observed in 70% of patients, dominated by incus destruction (45%), followed by malleus involvement (10%) and complete ossicular chain destruction (15%). The middle ear mucosa was judged inflammatory in more than half of the cases, and fibro-adhesive changes were described in 25%.
Canal wall up tympanoplasty was performed in 65% of patients, while the canal wall down technique was used in 35% of cases, primarily for extensive cholesteatomatous forms. Ossicular reconstruction was necessary in 48% of cases, using a PORP (22%), a TORP (18%), or an autologous ossicular graft (8%) based on the condition of the chain and the SAMEO-ATO classification.
Post-operative follow-up, with a mean duration of 12 months, showed satisfactory anatomical results in the majority of cases. Complete tympanic membrane healing was achieved in 83.3% of patients, while persistent tympanic membrane perforation was observed in 10%, and cholesteatoma recurrence in 6.7%. The stability of the operative cavity was judged good in 91.7% of cases, reflecting an overall efficacy of the surgical techniques employed.
Functionally, post-operative audiometric results revealed a notable improvement in hearing gain. The mean hearing loss improved from 42.1 dB to 29.8 dB, and the mean air-bone gap decreased from 32.7 dB to 20.6 dB, representing a statistically significant mean improvement of 12.1 dB (p < 0.05). An auditory improvement greater than 10 dB was achieved in 60% of patients, while 30% showed stable hearing and 10% experienced worsening. The best functional results were observed in patients with non-cholesteatomatous COM, an intact ossicular chain, and who underwent canal wall up tympanoplasty (p < 0.05).
Statistical analysis identified several significant prognostic factors. The type of otitis (cholesteatomatous vs. non-cholesteatomatous, p = 0.018), ossicular integrity (p = 0.022), the surgical technique used (p = 0.034), and the absence of post-operative complications (p = 0.041) were correlated with better hearing recovery. In contrast, age, sex, side of involvement, and the presence of initial otorrhea did not have a statistically significant influence on the results (p > 0.05).
Overall, the results of this series confirm the good efficacy of tympanoplasty surgery in the treatment of chronic otitis media, with durable anatomical preservation and notable functional improvement, particularly in non-cholesteatomatous forms and cases with preserved ossicles.
Discussion:
Chronic otitis media (COM) remains a major public health problem in developing countries due to its high prevalence, functional impact, and the risk of loco-regional or intracranial complications [1,2]. Its slow and insidious progression often leads to irreversible damage of the mucosa and the ossicular chain, responsible for a mixed or conductive hearing loss [3,4].
In our series, the mean age of patients was 33.9 years, aligning with results in the literature where the peak prevalence is generally between the third and fourth decades [5,6]. This distribution reflects the prolonged course of the disease and the often delayed access to specialized care. The slight female predominance observed (sex ratio = 0.9) is consistent with several African and Asian studies [7,8], although no clear hormonal or behavioral factor has been demonstrated.
Clinically, chronic otorrhea and hearing loss were the two main reasons for consultation, found in 85% and 80% of cases respectively. These results are comparable to those reported by Ralli et al. [9] and Aouad et al. [10], who describe otorrhea in over 80% of COM cases. These manifestations reflect the inflammatory and suppurative nature of the pathology, often sustained by a polymicrobial infection.
The etiopathogenic distribution in our series shows a slight predominance of non-cholesteatomatous forms (53.3%) over cholesteatomatous forms (46.7%). This trend is consistent with the international literature [11–13], where the non-cholesteatomatous form remains the most frequent, although the cholesteatomatous form is the most aggressive. Cholesteatoma is a destructive lesion characterized by the presence of keratinizing epithelium invading the middle ear spaces and capable of eroding bony structures, particularly the ossicular chain [14].
Table 1: The different reasons for consultation in our series and in the literature.
|
|
CHANDLER [2] |
MARTEL [24] |
RACHIDI [26] |
BEN CHEIKH [27] |
BEN GARMORA [28] |
CHNITIR [29] |
Our series |
|
Otalgia |
100 %
|
100 %
|
100 %
|
100 %
|
100 %
|
100 %
|
100 %
|
|
Otorrhea |
77 %
|
100 %
|
100 %
|
100 %
|
100 %
|
97 %
|
94,4 %
|
|
Facial palsy |
32 %
|
18 %
|
66 %
|
20 %
|
18 %
|
11 %
|
50 %
|
|
Hypoacusis |
- |
18 %
|
- |
- |
45 %
|
53 %
|
44,4 %
|
In our study, ossicular involvement was found in 70% of cases, dominated by destruction of the incus (45%). These figures align with those of Tos and Lau [15] and Palva et al. [16], who report ossicular involvement in 65% to 80% of operated cholesteatomas, with the incus being the most fragile and most exposed to enzymatic erosion.
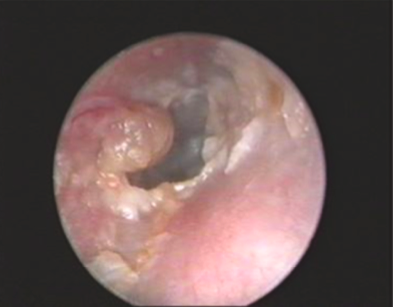
Figure 1: Granulation tissue in the external auditory canal on otoscopy.
Therapeutically, canal wall up tympanoplasty was the most frequently performed technique (65%), preferred for non-cholesteatomatous forms and limited cholesteatomas. This technical choice allows for better anatomical preservation and a lower recurrence rate [17,18]. Canal wall down techniques (35%) were reserved for extensive cholesteatomas, confirming the recommendations of the European Academy of Otology and Neurotology (EAONO) [19]. Ossicular reconstruction was performed in nearly half of the cases, mainly using PORP or TORP prostheses, as described by Dornhoffer [20].
The anatomical results obtained in our series are encouraging, with a tympanic membrane healing rate of 83.3%, a residual perforation in 10%, and a cholesteatoma recurrence in 6.7%. These results are comparable to those of Dornhoffer [20] and Quaranta et al. [21], who report anatomical success rates ranging from 80% to 90%. The maintenance of operative cavity stability in 91.7% of cases reflects good surgical technical mastery and regular post-operative follow-up.
Functionally, a mean hearing improvement of 12.1 dB was observed, with a significant reduction in the air-bone gap from 32.7 dB to 20.6 dB. These results are similar to those of Bento et al. [22] and Yung et al. [23], who report a mean hearing improvement of 10 to 15 dB after tympanoplasty. The hearing improvement of ≥10 dB observed in 60% of patients demonstrates the efficacy of tympano-ossicular restoration, particularly when the ossicular chain is preserved.
Statistical analysis identified several significant prognostic factors: the type of otitis (p = 0.018), ossicular integrity (p = 0.022), the surgical technique (p = 0.034), and the absence of complications (p = 0.041). These results corroborate the observations of Vartiainen [24] and Dornhoffer [20], who emphasize the determining influence of the ossicular status and surgical technique on the functional prognosis. In contrast, age, sex, and side of involvement did not show a significant influence, consistent with the conclusions of Quaranta et al. [21].
Finally, the comparison between cholesteatomatous and non-cholesteatomatous forms shows a clear difference in terms of hearing recovery, with the best performance obtained in non-cholesteatomatous COM. This finding, already reported by Glasscock et al. [25], is explained by the lesser ossicular destruction and better preservation of the middle ear mucosa in these forms.
Thus, our results confirm that the anatomical and functional prognosis of COM depends on the etiology, the ossicular status, and the technical choice, while underscoring the importance of early diagnosis and prolonged follow-up to prevent recurrences and improve hearing rehabilitation.
Conclusion:
Chronic otitis media remains a frequent and potentially disabling condition, whose surgical treatment aims both to eradicate disease in the ear and to restore hearing. The results of our series confirm that the anatomical and functional prognosis depends primarily on the type of otitis, the condition of the ossicular chain, and the surgical technique used. Non-cholesteatomatous forms and canal wall up tympanoplasties offer the best auditory and anatomical outcomes. Early management, combined with rigorous post-operative follow-up, remains essential to reduce the risk of recurrence and optimize functional recovery.