Aditum Journal of Clinical and Biomedical Research
OPEN ACCESS | Volume 8 - Issue 1 - 2026
ISSN No: 2993-9968 | Journal DOI: 10.61148/2993-9968/AJCBR
Ahmed N. Ghanem
Retired Consultant Urologist and Independent Investigator Masoura University, Faculty of Medicine, Egypt.
*Corresponding Author: Ahmed N. Ghanem, Retired Consultant Urologist and Independent Investigator Masoura University, Faculty of Medicine, Egypt.
Received: June 16, 2021
Accepted: June 21, 2021
Published: June 28, 2021
Citation: Ahmed N. Ghanem. (2021) “How and Why Starling’s law is killing ARDS patients in surgical practice in hundreds of thousands per year?.”, Aditum Journal of Clinical and Biomedical Research, 2(5); DOI: http;//doi.org/06.2021/1.1047.
Copyright: © 2021 Ahmed N. Ghanem. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly Cited.
Substantial, powerful and affirmative evidence currently exist both in articles and books [1-8] that demonstrates Starling’s law for the capillary-interstitial fluid (ISF) transfer is wrong and is responsible for the death of hundreds of thousands of patients who suffer from the acute respiratory distress syndrome (ARDS) each year. This concept and the questions of the title occurred to me in 1981 after I attended postmortem examinations on 3 patients who died of the transurethral resection of the prostate (TURP) syndrome. It was clear to me that these patients died of internal drowning as result of massive volumetric overload (VO) used for resuscitation of shock and was retained in their bodies. When I asked the pathologist why does not, he mention that retained VO in his report? He replied: “because it offends treating physicians”? I felt so strongly about it that I wrote a letter to the late great professor of physiology Eric Neil and author of Sampson Wright Textbook of Physiology later in 1983. He nicely replied in handwritten letter as he was in retirement asking: Why and how may Starling’s law cause death of patients?
Introduction:
To find the answers for these questions it took me a career lifelong of 40-years of investigations that started in 1981 by doing the physics study on the porous orifice (G) tube concluded in 1983-4. The clinical prospective cohort study on the TURP syndrome was done at mid-eighties. Having resolved the puzzle of TURP syndrome, I wrote my first essay theory on ARDS being induced by VO was sent it to the Lancet. My MD Thesis on the TURP syndrome was accepted in November 1988. This long journey of scientific research investigations has culminated in the publications of >100 articles and 8 books, 6 are published [1-6] and 2 remained [7, 8]. The investigations revealed 12 new scientific discoveries in physics, physiology and medicine [9]. The new scientific discoveries of the 20th and 21st centuries [2, 9] are:
Physics Discoveries:
The hydrodynamics of the porous orifice (G) tube [10-13]
The Tree Branching Law (TBL) [14].
Physiological Discoveries:
Proving Starling’s law for the capillary- ISF is wrong and providing the correct replacement of the magnetic field like fluid hydrodynamics of the G tube [10-12] (Figure 1).
The TBL Correct two widely received misconceptions on capillary physiology [8, 14]. It states that: “The trunk of a branching tree does not, and cannot, give rise to branches that have sum of all its cross-section areas larger than its own”. In other words: “The sum of all tree branches’ cross-section areas is less than its own trunk.” It applies to both green trees and the red tree of aorta and blood vessels. The two misconceptions are:
Biochemical Discoveries:
Resolving the puzzle of acute dilution hyponatraemia and the TURP syndrome identifying its path-aetiology and finding a successful curative lifesaving therapy for it: The Hypertonic Sodium Therapy (HST) of 5%NaCl and/or 8.4%NaCo3 [7, 15-18].
Revealing the effects of volume kinetics on the cardiovascular system on inducing volumetric overload shocks (VOS) type-1 (VOS-1) by sodium-free fluids of Glycine absorption and 5%Glucose infusion and VOS-2 by sodium-based fluids that include blood, plasma and saline.
Medical Discoveries:
Discovering two new types of cardiovascular shocks: the volume kinetic shocks or the volumetric overload shocks (VOS) [1, 19, 20] of type one induced by sodium-free fluid VO characterized with dilutional hyponatraemia, and type 2 induced by sodium-based fluid retention that have little or no serum markers [19, 20] (Figures 2, 3).
Resolving the puzzle of ARDS by identifying its exact patho-aetiology as caused by VOS and a successful lifesaving therapy of HST [5, 21, 22].
Resolving the puzzle of the TURP syndrome discovering its link with ARDS and finding the successful lifesaving therapy for it similar to that of acute hyponatraemia. Table 1 shows high statistical significance of VO in inducing VOS and causing ARDS as shown in (Figures 2, 3).
Discovering the bridge connecting the physics, physiology, biochemistry, and medicine [22].
To link the basic physics scientific discoveries to its physiological relevance and clinical significance, the reported evidence is highlighted here. Starling’s law being wrong dictates the faulty rules on current fluid therapy in shock management, misleading physicians into giving too much fluid during the resuscitation of septic, hemorrhagic and hypovolemic shock. This is similar to treating the hyponatraemic shock of the TURP syndrome with further volume expansion [3, 6]. This induces VOS [19, 20] that cause ARDS [21, 22]: Both are iatrogenic complications of fluid therapy in shock management [6]. The exact patho-etiology of VOS and ARDS has been identified and a successful 100% preventable and curable therapy of HST is advanced [5, 21, 22]. The new scientific basis of fluid therapy in shock management has been written [6].
The studies performed are: Discovering and reporting the hydrodynamics of the porous orifice (G) tube built on the capillary ultrastructure of having a narrow pre-capillary sphincter and a porous wall. This demonstrated the rapid magnetic field like fluid circulation around the G tube between fluid in its lumen and that surrounding it (Figure 1). The tree branching law discovered lately dispels two major and widely received misconceptions on capillary cardiovascular physiology [8, 14]. The physiological study was done on the hind limb of slaughtered sheep [8, 23]. Running both saline and albumin through the artery and later the vein demonstrated that edema occurred with both fluids when run through the vein but not through the artery. This indicated that the capillary works as G tube, not Poiseuille’s tube, in which the hydrostatic pressure causes suction and the oncotic pressure of plasma proteins does not work. The clinical studies were the prospective cohort study on 100 TURP surgery patients [24] of whom 10 developed the TURP syndrome, and the case series of 23 TURP syndrome patients [25] (Table 2) who have similar clinical picture to ARDS (Table 3).
My research has not only identified the problems but also find the solutions for it. In case of the above mentioned TURP syndrome, Hyponatraemia and ARDS the exact precise patho-aetiology was found and 100% successful lifesaving preventative and curative therapy is advanced. Now is the time to say Goodbye Starling’s law and hello G tube [26] and to start saving the lives of hundreds of thousands of ARDS patients per year all over the world.
Figures and Legends:
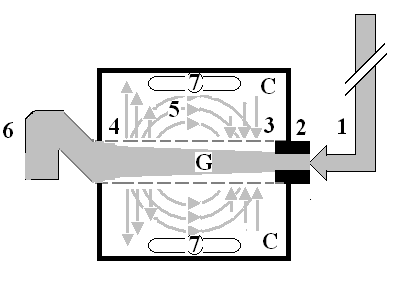
Figure 1: shows a diagrammatic representation of the hydrodynamic of G tube based on G tubes and chamber C. This 37-years old diagrammatic representation of the hydrodynamic of G tube in chamber C is based on several photographs. The G tube is the plastic tube with narrow inlet and pores in its wall built on a scale to capillary ultra-structure of precapillary sphincter and wide inter cellular cleft pores, and the chamber C around it is another bigger plastic tube to form the G-C apparatus. The chamber C represents the ISF space. The diagram represents a capillary-ISF unit that should replace Starling’s law in every future physiology, medical and surgical textbooks, and added to chapters on hydrodynamics in physics textbooks. The numbers should read as follows:
1.The inflow pressure pushes fluid through the orifice
2. Creating fluid jet in the lumen of the G tube**.
3. The fluid jet creates negative side pressure gradient causing suction maximal over the
Proximal part of the G tube near the inlet that sucks fluid into lumen.
4. The side pressure gradient turns positive pushing fluid out of lumen over the distal
part maximally near the outlet.
5. Thus, the fluid around G tube inside C moves in magnetic field-like circulation (5)
taking an opposite direction to lumen flow of G tube.
6. The inflow pressure 1 and orifice 2 induce the negative side pressure creating the dynamic G-C circulation phenomenon that is rapid, autonomous, and efficient in moving fluid and particles out from the G tube lumen at 4, irrigating C at 5, then sucking it back again at 3,
7. Maintaining net negative energy pressure inside chamber C.
**Note the shape of the fluid jet inside the G tube (Cone shaped), having a diameter of the inlet on right hand side and the diameter of the exit at left hand side (G tube diameter). I lost the photo on which the fluid jet was drawn, using tea leaves of fine and coarse sizes that run in the center of G tube leaving the outer zone near the wall of G tube clear. This may explain the finding in real capillary of the protein-free (and erythrocyte-free) sub-endothelial zone in the Glycocalyx paradigm (Woodcock and Woodcock 2012) [3]. It was also noted that fine tea leaves exit the distal pores in small amount maintaining a higher concentration in the circulatory system than that in the C chamber- akin to plasma proteins.
Photographs:

Figure 2: shows the means and standard deviations of volumetric overload in 10 symptomatic patients presenting with shock and hyponatraemia among 100 consecutive patients during a prospective study on transurethral resection of the prostate. The fluids were of Glycine absorbed (Gly abs), intravenously infused 5% Dextrose (IVI Dext) Total IVI fluids, Total Sodium-free fluid gained (Na Free Gain) and total fluid gain in liters.
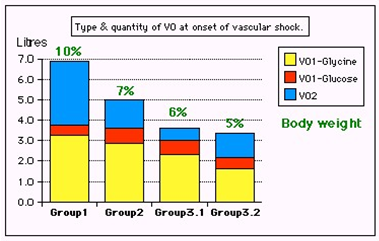
Figure 3: shows volumetric overload (VO) quantity (in liters and as percent of body weight) and types of fluids. Group 1 was the 3 patients who died in the case series as they were misdiagnosed as one of the previously known shocks and treated with further volume expansion. Group 2 were 10 patients from the series who were correctly diagnosed as volumetric overload shock and treated with hypertonic sodium therapy (HST). Group 3 were 10 patients who were seen in the prospective study and subdivided into 2 groups; Group 3.1 of 5 patients treated with HST and Group 3.2 of 5 patients who were treated with guarded volume expansion using isotonic saline
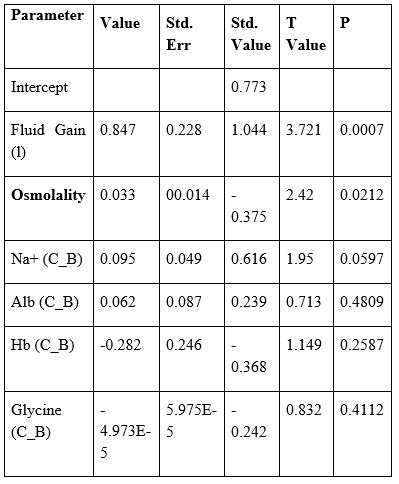
Table 1: shows the multiple regression analysis of total per-operative fluid gain, drop in measured serum osmolality (OsmM), sodium, albumin, Hb and increase in serum glycine occurring immediately post-operatively in relation to signs of the TURP syndrome. Volumetric gain and hypo osmolality are the only significant factors.
|
1 |
Gr1 |
Gr2 |
Gr3 |
Gr3.1 |
Gr3.2 |
Normal Units |
||
|
2 |
Number of patients 3 |
10 |
10 |
5 |
5 |
mean |
||
|
3 |
Age 71 |
70 |
75 |
72 |
78 |
72 Years |
||
|
4 |
Body weight (BW) 69 |
70 |
68 |
71 |
65 |
69 Kg |
||
|
5 |
Postoperative serum solute concentration |
|
Preoperative |
|||||
|
6 |
Osmolality |
271 |
234 |
276 |
282 |
271 |
292 |
Mosm/1 |
|
7 |
Na+ |
110 |
108 |
120 |
119 |
121 |
139 |
Mmol/1 |
|
8 |
Ca++ |
1.69 |
1.79 |
1.85 |
1.84 |
1.86 |
2.22 |
'' |
|
9 |
K+ (P<.05) |
5.6 |
4.8 |
5.0 |
4.9 |
5.0 |
4.46 |
'' |
|
10 |
Co2 (P=.002) |
23.0 |
23.0 |
25.5 |
24.0 |
26.4 |
27.30 |
'' |
|
11 |
Glucose |
13.2 |
17.3 |
16.4 |
15.9 |
16.9 |
6.20 |
'' |
|
12 |
Urea (P=.0726) |
26.5 |
9.0 |
6.6 |
6.8 |
6.4 |
6.7 |
'' |
|
13 |
Bilirubin (P<.05) |
19 |
16 |
8 |
6 |
9 |
7 |
'' |
|
14 |
AST |
124 |
32 |
20 |
18 |
21 |
20 |
'' |
|
15 |
Protein |
43 |
52 |
48 |
44 |
52 |
62 |
g/l |
|
16 |
Albumin |
23 |
30 |
30 |
28 |
32 |
39 |
'' |
|
17 |
Hb (P=.0018) |
119.3 |
127.9 |
114.5 |
105.2 |
123.8 |
123.8 |
'' |
|
18 |
WCC (P<.005) |
18.9 |
16.2 |
7.5 |
7.8 |
7.2 |
8.0 |
per HPF |
|
19 |
Glycine |
|
|
10499 |
|
|
293 |
µmol/1 |
|
20 |
Therapy |
CT |
HST |
Randomized: |
HST |
CT© |
|
|
|
21 |
Outcome |
Death |
Full Recovery |
|
Full Reccovery |
Morbidity |
|
|
Table 2: Shows the mean summary of data, therapy and outcome comparing the 3 groups of 23 case series patients whose VO is shown in (Figure 3). Groip-1 was the 3 patients who died and had post mortem examination, Group-2 were a series of severe TURP syndrome cases successful ly treated with hypertonic sodium therapy (HST), and Group-3 were 10 patients encountered in the prospective study who were randomized between HST (3.1) and conservative treatment (CT) (3.2). The significant changes of serum solute contents are shown in bald font with the corresponding p- value. Most of the patients showed manifestation of ARDS of which the cerebral manifestation predominated, being on initial presentation (Regional Anesthesia) and representation of VOS 1 (General Anesthesia). However, most patients were given large volume of saline that elevated serum sodium to near normal while clinical picture became worse. They suffered VOS2 that caused ARDS. The VO of patients to whom these data belongs is shown in (Figure 3), Please note the elevation of urea and anuria of Group 1 who died indicated AKI. Elevations of Bilirubin and AST indicated hepatic dysfunctions. White cell count (WCC) elevation indicated inflammatory response of VOS 2 in ARDS or SIRS in the absence of sepsis
|
Cerebral |
Cardiovascular |
Respiratory |
Renal |
Hepatic & GIT |
|
Numbness |
Hypotension |
Cyanosis. |
Oliguria |
Dysfunction: |
|
Tingling |
Bradycardia |
FAM4 |
Annuria8 |
Bilirubin ↑ |
|
SBB1 |
Dysrhythmia |
APO)5 |
Renal failure |
SGOT ↑ |
|
COC2 |
CV Shock* |
RA6 |
or |
Alkaline |
|
Convulsions |
Cardiac Arrest |
Arrest |
AKI9 |
Phosph. |
|
Coma |
|
CPA7 |
Urea ↑ |
GIT |
|
PMBCI 3 |
Sudden Death |
Shock lung |
Creatinine ↑ |
symptoms. |
|
|
|
ARDS$ |
|
DGR10 |
|
|
|
|
|
Paralytic ileus |
|
|
|
|
|
Nausea & Vomiting. |
Table 3: shows the manifestations of VOS 1 of the TURP syndrome for comparison with ARDS manifestations induced by VOS2. The manifestations are the same but one vital organ-system may predominate.
Table Abbreviation:
SBB1: Sudden Bilateral Blindness
COC2: Clouding of Consciousness
MBCI3: Paralysis mimicking bizarre cerebral infarctions, but is recoverable on instant use of HST of 5%NaCl and/or NaCO3, and so is coma and AKI
FAM4: Frothing Around the Mouth
APO5: Acute Pulmonary Oedema;
RA6: Respiratory Arrest;
CPA7: Cardiopulmonary Arrest;
ARDS$: Occurs later on ICU
Annuria8: That is unresponsive to diuretics but responds to HST of 5%Ncl and/or 8.4%NaCO3;
AKI9: Acute Kidney Injury.
Also occurs the excessive bleeding at the surgical site
DGR10: Delayed Gut Recovery;
CV Shock*: Cardiovascular shock
Excessive bleeding may occur at the surgical site and leukocytosis occurred in the absence of sepsis and septic shock.