International Surgery Case Reports
OPEN ACCESS | Volume 8 - Issue 1 - 2026
ISSN No: 2836-2845 | Journal DOI: 10.61148/2836-2845/ISCR
Imran Pathan 1, Ravi Kumar Chittoria 2*, Chirra Likhitha Reddy 3, Padmalakshmi Bharathi Mohan 4, Shijina K 5, Nishad K 6, Neljo Thomas 7, Madhusudan 8, Girish Mirajkar 9, Madan S 10.
1,3,4,5,6,7,8,9 Senior Resident Department of Plastic Surgery Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, India-605006
2 Professor Department of Plastic Surgery, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, ndia-605006
10 Junior resident Department of Surgery Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry India-605006
*Corresponding author: Ravi Kumar Chittoria, Professor Department of Plastic Surgery Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER) Pondicherry, India
*Corresponding author: Ravi Kumar Chittoria, Professor Department of Plastic Surgery Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER) Pondicherry, India
Received date: February 01, 2021
Accepted date: February 05, 2021
published date: February 10, 2021
Citation: Pathan I, Ravi K Chittoria, Chirra L Reddy, Padmalakshmi B Mohan, Shijina K. “Role of Closed Incision Negative Pressure Wound Therapy in Electrical Burn Injury”. International Surgery Case Reports, 1(1); DOI: http;//doi.org/03.2021/1.1001.
Copyright: © 2021 Ravi Kumar Chittoria. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Electrical burn may cause deep burn injury. These injuries may be complicated by surgical site infection (SSI). Various methods have been described in literature to prevent this complication. Recently application of negative pressure to a surgically closed wound has also emerged as a way of preventing this complication. The commercially available devises do exist for such type of dressings but are usually too costly. In this article we share our experience of using negative pressure wound therapy ( NPWT) in cost effective manner.
Introduction
Negative pressure wound therapy has changed the way by which acute and chronic wounds are managed.[1,2] Various randomized control trials have established its role in the management of chronic and acute wounds.3 Traditionally, after the primary closure of the wound, the incision site is covered with an occlusive or semi-occlusive dressing. In recent years negative pressure therapy also has been tried for the wound that has been surgically closed primarily, especially in cases that are at high risk of surgical site infection (SSI).[4, 5] In this article we share our experience of closed incision negative pressure wound therapy (ci-NPWT) in an electrical burn injury case.
Methodology
This study was conducted in the department of plastic surgery in a tertiary care centre. This study was conducted in January 2021. The patient was a 29 year male with an alleged history of electrical burn injury with a wound on the left eyebrow (Figure-1).
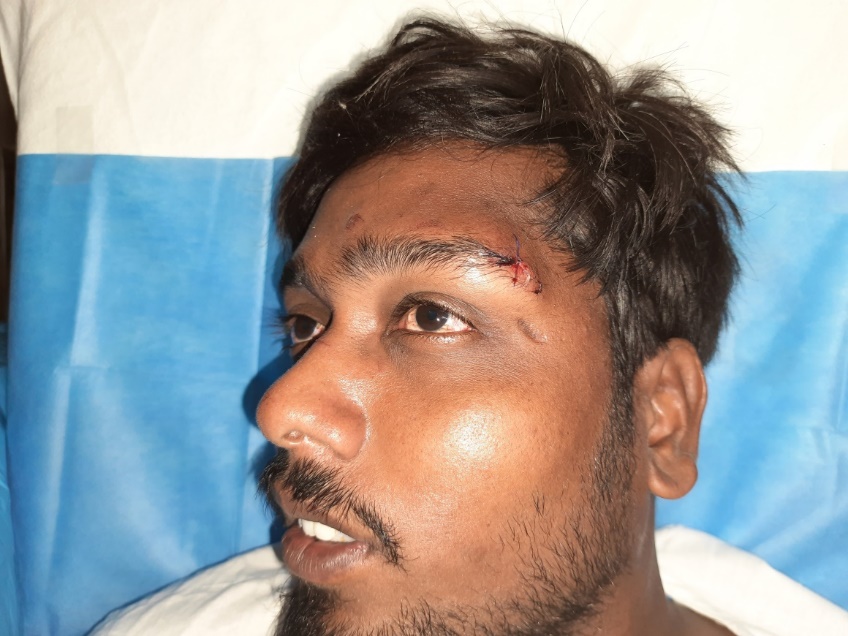
Figure 1: sutured wound
As the patient was at high risk of SSI, a decision was made to apply a customized NPWT. An informed and written consent was taken and departmental ethical approval was taken. A sterile sponge was taken of appropriate size. A small-caliber suction tube with multiple holes was passed through it. A single layer of non-adherent gauze was placed on the closed incision site. The sponge with suction tube in-situ was placed on the incision site. An adherent transparent occlusive dressing was placed. The continuous negative pressure of 100mm of Hg was applied for seven days (Figure-2).

Figure 2: closed incision site covered wit foam and transparent adhesive dressing
The patient was assessed daily for any systemic sign of infection. Daily inspection through transparent dressing was done to look for any soakage, erythema of skin localized tenderness, or swelling. The dressing was removed after 7 days and the operative site was assessed.
Result
After application of ci-NPWT, a daily assessment was done, no systemic or local sign of infection was noted. The dressing was removed and the surgical site was inspected after seven days. The wound was healed well (Figure-3).

Figure 3: well healed wound without any complication
Sutures were removed on the next day. No wound dehiscence was noted.
Discussion
Despite advances in surgical practice, surgical site infections (SSI) are frequent complications in patients who undergo surgery. The cause of SSI may be pre-operative, intraoperative, and postoperative.[6] There are multiple factors that predispose the patient to SSI like- malnutrition, anemia, hypoproteinemia, smoking, DM, etc. Preventive measures should be taken at every step to control it. NPWT has recently emerged as a strategy to reduce the SSI, particularly in high-risk patients.[7,8] Apart from this, the wounds that are closed under tension may also be benefited from ci-NPWT.
Negative pressure wound vacuum therapy has an established treatment for open surgical incisions following infection or breakdown. Recently there has been been the focus of new investigation in its use in closed surgical site. The first publication regarding closed incisions using NPWT (ciNPT) was in 2006 when Gomoll et al published his results utilizing a similarly modified incisional dressing. Various mechanisms has been proposed for NPWT [9, 10, 11]
Macroscopic Effects of NPWT
Creates and maintains a moist wound environment, shortens time to wound closure
Reduces wound edema
Helps limit seroma formation
Promotes more robust granulation tissue when compared to traditional occlusive dressing
Stimulates wound contracture through macro deformation
NPWT stabilizes healing tissues through a bolstering Effect
Provides appositional forces to both superficial and deeper healing tissues
Reduces size and complexity of the healing wound
Microscopic Effects of NPWT
Increased expression of VEGF, IL-8 VEGF gradient increases toward the wound
Vigorous angiogenesis in a parallel fashion, oriented toward the wound compared to fewer tortuous new vessels observed in controls
Increases blood flow around the periphery of the wound; improves local delivery of antibiotics
Stimulates cell proliferation through micro-deformation
Decreases local blood flow in those tissues in closest proximity to the ROCF
Removal of cytokines and other soluble inhibitors of wound healing (e.g., matrix metalloproteinases)Changes in the colonizing flora of the wound, may increase or not affect overall bacterial load
Increased neovascularization
There are commercially available devices for ci-NPWT. These devices are expensive for routine use in the hospitalized patient. We have used a simple way of applying ci-NPWT cost-effectively.
Conclusion
SSI is a common problem; all preventive measures should be taken. In this study, we found that ci-NPWT helps in preventing SSI in high-risk cases. But since it is a single case study, a definite conclusion cannot be made. Large randomized control trials are required to confirm the efficacy of NPWT in the surgically closed wound.
Conflicts of interest: None.
Declarations Authors’ contributions: All authors made contributions to the article
Availability of data and materials: Not applicable.
Financial support and sponsorship: None.
Consent for publication: Not applicable.